


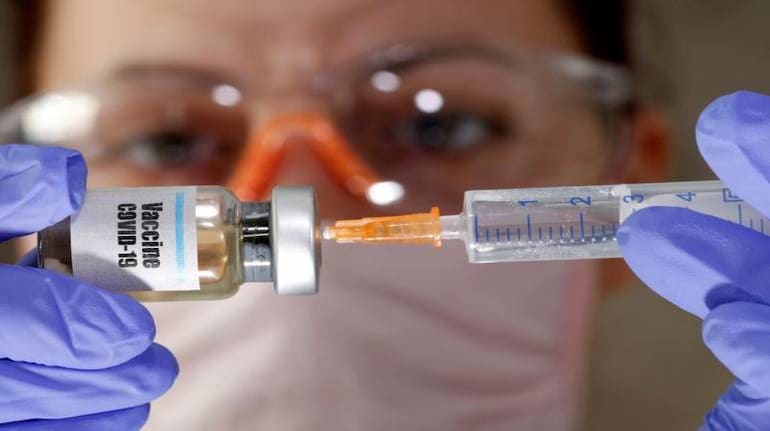
British-Swedish drug maker AstraZeneca and the University of Oxford on November 23 said that the Coronavirus vaccine they are developing is 70.4 percent effective, on an average, in preventing COVID-19, as per the interim analysis of its late-stage clinical trials conducted in the UK and Brazil.
The positive data makes a strong case for AstraZeneca's India partner Serum Institute of India to seek licence for its potential vaccine, Covishield, from the Indian government.
But AstraZeneca and University of Oxford data have intrigued many experts.
Why one-and-a-half dose is better than two?Preliminary results on the AstraZeneca vaccine were based on a total of 131 COVID-19 cases in a study involving 11,636 participants. In Brazil, two full doses of the vaccine were given one month apart, involving 8,895 participants and appeared to be 62 percent effective, while half dose, followed by a full dose, was given in UK, involving a much smaller subset of 2,741 participants. Here the vaccine demonstrated 90 percent effectiveness. The average efficacy of both the dosing regimens put together was 70.4 percent.
In fact, the clinical trial protocol of Serum Institute of India, which is conducting phase 2/3 trials for Covishield, also follows the Brazil protocol, with two full 0.5 ml doses given one month apart.
This has raised questions on why one-and-a-half dose is more effective than two full doses. Dr Gagandeep Kang, India's leading expert on vaccines and Professor at the Department of Gastrointestinal Sciences at Christian Medical College, Vellore, said in the microblogging site Twitter that possibly less adenovirus first time around resulted in lower immune response that did not block the response to the second dose.
Follow Moneycontrol's COVID-19 Vaccine Tracker here."Prime-boost is complicated. Selection of antigen, type of vector, delivery route, dose, adjuvant, boosting regimen, the order of vector injection, and the intervals between different vaccinations influence outcome. Is it at play here? Possible. But the bottom line is AstraZeneca's vaccine works well. Can we improve its performance? Very possible, there is a lot we do not understand about human immunology. The pandemic is making us learn and fast," Kang said.
Prime-boost refers to first dose. The Oxford vaccine uses re-engineered version of Chimpanzee adenovirus vector fused with genetic material of the SARS-CoV-2 spike protein to elicit immune response.
The official Twitter handle of Russia's Sputnik V vaccine rival to AstraZeneca took potshots at the latter’s vaccine. "The possible reason for 62 percent efficacy of AstraZeneca’s full dose regimen is that immunity to Chimpanzee adenoviral vector from the first shot makes the second shot ineffective. Sputnik V addresses this issue by using two different human adenoviral vectors for two shots," it says.
Sputnik V vaccine claims 91.4 percent efficacy in second interim analysis on day 28 after first dose.
"If you say the lesser dose vaccine is producing better efficacy than the full dose, and that too for a small subset of participants, then it is cherry-picking," said an executive at vaccine a company, who didn't want to be named.
AstraZeneca's interim analysis data exceeds the 50 percent primary efficacy endpoint set by Indian drug regulator, the Central Drugs Standard Control Organisation (CDSCO), as part of its draft regulatory guidelines for COVID-19 vaccines. The vaccine is also safe.
Please read here on why Covishield is better suited to India.Why serendipity?According to AstraZeneca and University of Oxford scientists, the smaller dose wasn't part of the original design, but was administered by accident during a trial of the experimental COVID-19 vaccine. This generally could be a cause of embarrassment, but a Reuters report quoting Mene Pangalos, the head of AstraZeneca’s non-oncology research and development, called the error as "serendipity”.
Pangalos said that around the time when AstraZeneca was initiating its partnership with Oxford at the end of April, university researchers were administering doses to trial participants in Britain. They soon noticed expected side effects such as fatigue, headaches or arm aches were milder than expected.
“So we went back and checked ... and we found out that they had under-predicted the dose of the vaccine by half,” Pangalos was quoted in the Reuters report.
The AstraZeneca and Oxford University researchers decided to continue with the half dose and administer the full dose booster shot at the scheduled time in the UK.
Kang added that populations differ in prior exposure, current exposure, genetic background and a host of other factors, and said much data is needed to understand whether this is just a UK/Brazil difference.
Discover the latest Business News, Sensex, and Nifty updates. Obtain Personal Finance insights, tax queries, and expert opinions on Moneycontrol or download the Moneycontrol App to stay updated!
Find the best of Al News in one place, specially curated for you every weekend.
Stay on top of the latest tech trends and biggest startup news.