


Drug-resistant pathogens are the stuff horror movies are made of. But this is slowly becoming a reality as a long list of these harmful microbes begin to mutate or emerge unaffected by long-standing antibiotics.
Since the discovery of penicillin by Alexander Fleming, modern medicine has saved millions of lives. But more and more of these pathogens fighting back, and breakthroughs in treatment coming coming few and far between, the threat is very real.
The latest on the list? Candida auris; also known as C. auris.
What is it?
A deadly fungus with a high resistance to the most commonly available anti-fungal drugs and long incubation period, C. auris has emerged as a major global health threat.
The fungus is highly infectious and with a mortality rate of 30-60 percent, as per a Centers for Disease Control and Prevention (CDC) factsheet. Amplifying the threat is low knowledge and delayed detection of the bug.
The CDC has identified three major reasons for concern to treat C. auris infections:
- It is often multidrug-resistant, meaning that it is resistant to multiple antifungal drugs commonly used to treat Candida infections.
- Difficult to identify with standard laboratory methods, and it can be misidentified in labs without specific technology, which may lead to inappropriate management.
- Has caused outbreaks in healthcare settings through contact with contaminated environmental surfaces or equipment, or from person to person. For this reason, it is important to quickly identify C. auris in a hospitalised patient so that healthcare facilities can take special precautions to stop its spread.
Detection and threat
Considered an emerging pathogen because of the increasing numbers of infections, C. auris has been identified in multiple countries since it was recognised.
The CDC report noted that patients who are infected with the fungus are also usually affected by other diseases, making it difficult to detect. Symptoms such as fevers and chills that do not go away after persistent treatment with antibiotics taken for a suspected bacterial infection should ring alarm bells for a possible C. auris infection.
Identified in 2009 in Japan, followed by two cases in South Korea in 2011, and in India the same year, it has now spread to at least 30 countries over a span of just 10 years. ''Because identification of C. auris requires specialised laboratory methods, infections likely have occurred in other countries but have not been identified or reported,'' the CDC stated.
In India, as many as 200 cases have been reported in hospitals in the last two years alone and research has shown that the strain grows well at 40 degrees Celsius, which explains why tropical countries like India tend to offer a better place for such germs to spread, Mint reported.
The battleground is the intensive care units (ICUs) of hospitals, where the fungus finds ground to incubate and infect patients with lowered immunity. ''In some patients, this yeast can enter the bloodstream and spread throughout the body, causing serious invasive infections,'' the CDC factsheet added.
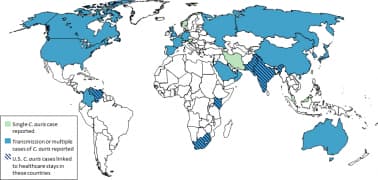
Countries from which Candida auris cases have been reported, as of March 31, 2019 Source: CDC
The first cases in India were detected by a team among 12 patients in two Delhi hospitals between 2011 to 2013. Leading the team was Anuradha Chowdhary from Vallabhbhai Patel Chest Institute, Delhi University, who told Mint that the fungus behaved like bacteria by cloning itself quickly and being easily transmittable. Chowdhary’s study found that of the 27 ICUs studied across the country, as many as 19 were affected by the fungus at different times during the period of the research.
Mint cited another paper published in the Journal of Antimicrobial Chemotherapy in 2017, which found that the number of C. auris infection cases was higher in public hospitals in North India.
In 2017, the Indian Council of Medical Research (ICMR) issued an advisory and mandated hospitals to report the occurrence of the fungus. ''But many labs do not have access to higher-end identification systems, the cases go unreported,'' Dr Joy Sarojini Michael of Christian Medical College (CMC), Vellore told the paper.
Prevention & treatment
The Mint report noted that as of now, three classes of anti-fungal drugs exist – azoles, echinocandin, and polyenes, and C. auris shows highest resistance (nearly 90 percent) to the first line of drugs; the level of resistance to the second line of drugs is around 5-7 percent.
The CDC factsheet points out that most C. auris infections are treatable with echinocandins. However, some C. auris infections have been resistant to all three main classes of antifungal medications, making them more difficult to treat and requiring multiple classes of antifungals at high doses.
Chowdhary told Mint that when it comes to treatment, the options are limited and no new antifungal drug has entered the market in the last 10 years.
While the prospect seems grim, simple preventive measures could go a long way. Once detected, the ICU and equipment must be properly disinfected and patients should be appropriately quarantined for treatment.
In countries like India, a little over one million modern medicine doctors to treat a population of 1.3 billion people and only around 10 percent working in the public health sector, the shut down of facilities detected to house the fungus would be an expensive ask.
Discover the latest Business News, Sensex, and Nifty updates. Obtain Personal Finance insights, tax queries, and expert opinions on Moneycontrol or download the Moneycontrol App to stay updated!
Find the best of Al News in one place, specially curated for you every weekend.
Stay on top of the latest tech trends and biggest startup news.