



The spread of the COVID-19 infection into the interior regions of the country might prove devastating despite the measures proposed by the Centre to create facilities to provide care to patients, distribute medicines and essential medical devices such as thermometer and pulse oximeter.
The ministry of health and family welfare in a note to states on May 16 had spelt out the standard operating procedure (SOP) for containing and managing the diseases. However, the effectiveness of the three-tier structure of Covid care centres, dedicated Covid health centres and dedicated Covid hospitals in peri-urban, rural and tribal areas proposed by the ministry depends on the existing healthcare infrastructure in rural areas.

The existing government-run healthcare infrastructure in rural areas is inadequate, under-equipped and understaffed. The number of health centres, doctors, nurses, lab technicians and other healthcare workers falls short of the numbers prescribed in the Indian Public Health Standards (IPHS), official data show. The shortage of doctors is acute – on average the community health centres that serve as hospitals have just about 20 percent of the required specialists including gynaecologists and paediatricians.
The SOP issued by the ministry requires that Covid care centres with a minimum of 30 beds be set up under the supervision of public health centres (PHC) and community health centres (CHC) for suspected and confirmed cases who cannot isolate at home. The PHCs, CHCs and sub-district hospitals are required to run dedicated Covid health centres with a minimum of 30 beds to provide care for patients clinically assigned as moderate while retaining non-Covid essential services.
What the Covid SOP mandates
Private hospitals can also be designated as dedicated Covid health centres. District hospitals and identified private hospitals are to be converted into dedicated Covid hospitals. The covid care centres are to be mapped dedicated Covid health centres and dedicated Covid hospitals for referring patients whose condition turn serious and the dedicated Covid health centre to the dedicated Covid hospitals.
The SOP envisages that care for patients at the Covid care centres will be provided by auxiliary nurse midwives and male multipurpose health workers with the support of ASHA/Anganwadi workers under the guidance of a health officer from the health and wellness centre created from transforming the subhealth centres and PHCs. Qualified Ayush doctors and final year Ayush and BSc (nursing) students are also proposed to be roped in. Every dedicated Covid health centres require more than one doctor, several nurses, pharmacists and other health workers.
Data lays bare shortfall
The question that begs an answer is whether rural India has enough health care centres, doctors, nurses, lab technicians and other health workers to lead the war against the spread of the virus. Official data is not very encouraging.
As things stand, India has a three-tiered healthcare infrastructure in rural areas, with the sub centres at the bottom of the pyramid and the CHCs that serve as hospitals at the top. The PHC acts as a link between the sub centres and the CHCs.
There were 1,57,411 sub centres, 24,855 PHCs and 5,335 CHCs across rural India as of March 2019. Data for the following fiscal years has not been published yet. A CHC serves an area of 500 sq km and a population of 1.66 lakh on average, a PHC an area of 120 sq km and a population of 35,567 and a sub centre an area of 19 sq km and a population of 5,616.
Data published by the Ministry of health and family welfare show understaffing to be a problem at health centres at every level and across states. Of the 1,57,411 sub centres as of March 2019, 7,821 had been upgraded to health and wellness centres under the Ayushman Bharat mission.
Of the 1,49,590 that continued as sub centres, 13,773 did not have an auxiliary nurse midwife or a female health worker, 81,007 did not have a male health worker and 5,757 had neither. The sub centres are not required to have doctors. That situation might have improved only marginally over the last two years.
Woeful deficit
The government data also shows that there was a 62 percent shortfall in male health workers against the requirement under the Indian Public Health Standards. The shortfall was about 70 percent or more in West Bengal, Rajasthan, Bihar, Tamil Nadu, Telangana and Uttar Pradesh. The shortfall in female health workers or auxiliary nurse midwives was a little under 3 percent.
Similarly, of the 24,855 PHCs, 8,242 had been converted into health and wellness centres. Of the 16,613 that continued as PHCs, 1,598 were without even a single doctor, 6,378 without a lab technician and 3,971 without a pharmacist.
Only 5,156 centres had a female doctor. Just 984 centres had more than four doctors while a majority - 8,463 - had just one doctor. Karnataka had the most single doctor run PHCs, followed by Uttar Pradesh, Bihar and Rajasthan. Chhattisgarh, Madhya Pradesh and Karnataka had the most number of PHCs didn’t have a doctor on the rolls.
The shortfall in the number of doctors in the PHCs against the requirement was 6 percent but it was as high as 59 percent in Chhattisgarh and 37 percent in Odisha. The shortfall in the number of nursing staff stood at 23 percent female health workers or auxiliary nurse midwives at 26 percent, female health assistants at 48 percent, male health assistants at 60 percent, pharmacists at 29 percent and laboratory technicians at 51 percent.
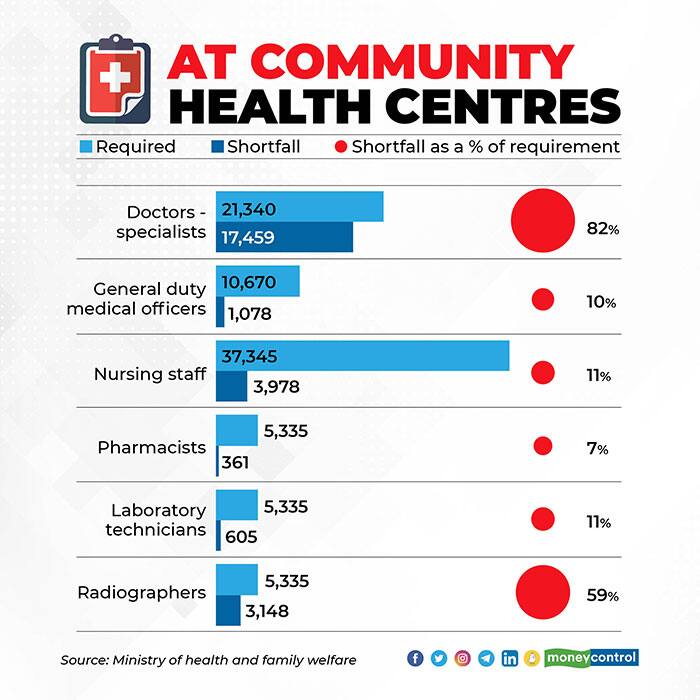
The shortfall of specialist doctors at the CHCs was estimated at 82 percent. Of a total of 21,340 physicians, surgeons, paediatricians, gynaecologists and obstetricians required at the CHCs to provide effective health care to the rural population, there were only 3,881 in position. Each of the 5,335 CHC is required to have doctors of the four specialisations.
In addition, they can have a dental surgeon. Most of these CHCs run on the strength of general duty medical officers. Each CHC is required to have two such doctors. The shortfall in their numbers was 10 percent at the end of March 2019.
There was a shortfall in the number of other health workers and technicians at the CHCs. The shortfall in the number of radiographers was 59 percent, pharmacists 7 percent, laboratory technicians 11 percent and nursing staff 11 percent.
The shortfall in the number of doctors at district hospitals was about 14 percent and at the sub-district and sub-divisional hospitals at 40 percent. The corresponding numbers for the shortfall of paramedical staff were 6 percent and 30 percent, respectively.
Given that there is a shortfall in the number of medical professionals, caregivers and technicians in rural areas, efforts of the Union and state governments to provide appropriate care to Covid patients looks certain to face many challenges.
The creation of makeshift care centres with oxygen beds will save many lives. The proposal to induct volunteers, final year students of medicine and nursing will help overcome some of the shortfalls temporarily but it may not be enough.
Discover the latest Business News, Sensex, and Nifty updates. Obtain Personal Finance insights, tax queries, and expert opinions on Moneycontrol or download the Moneycontrol App to stay updated!
Find the best of Al News in one place, specially curated for you every weekend.
Stay on top of the latest tech trends and biggest startup news.